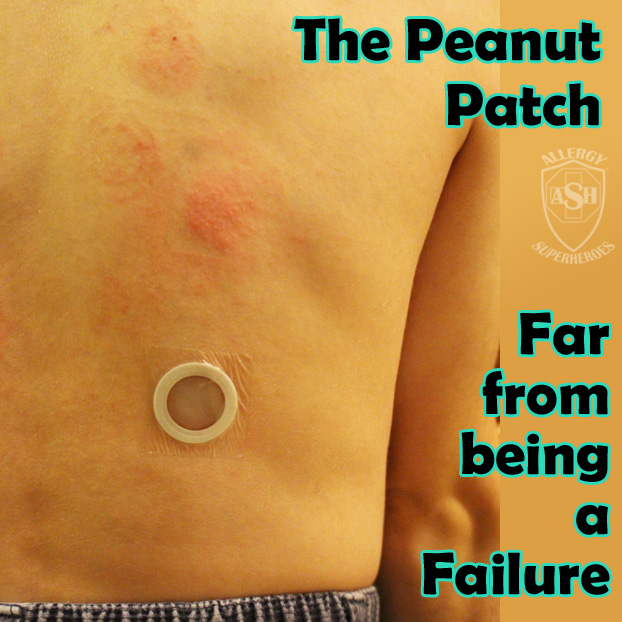
Following the Peanut Patch trial, we tried Kal on Oral Peanut Dosing. Read Part 1 for our experience participating in DBV Technology’s REALISE Peanut Patch Trial. For three and a half years, we followed the mundane pattern of “Patch On, Patch off.” Then it came time to end the trial.

Next Steps
Ever since we began the trial, I’ve wondered what we would do after it ended. All previous data says that allergen tolerance requires regular exposure. If exposure stops, tolerance disappears. So I knew that we would have to do something to maintain Kal’s tolerance once the trial was over. Assuming the patch worked and Kal gained tolerance.
Participating in clinical research, of course, has no guarantees. There’s no guarantee that the treatment will achieve the desired results. There’s no guarantee that you’ll be able to keep those results if they do appear. The study doctor said we’d have to cross that bridge when we came to it, because we had no way of knowing where we’d be when it was over.
When we began, there was even the possibility that the patch would be FDA approved before our trial was finished. If that happened, Kal might have been able to just continue using it, through his regular allergist. Unfortunately, with DBV’s setbacks and problems, that didn’t happen.
We had our “End of Treatment” visit on August 11, 2020. They removed the last patch (surprisingly, it was still on that day) and collected our study logs and unused patches. And then we discussed options.
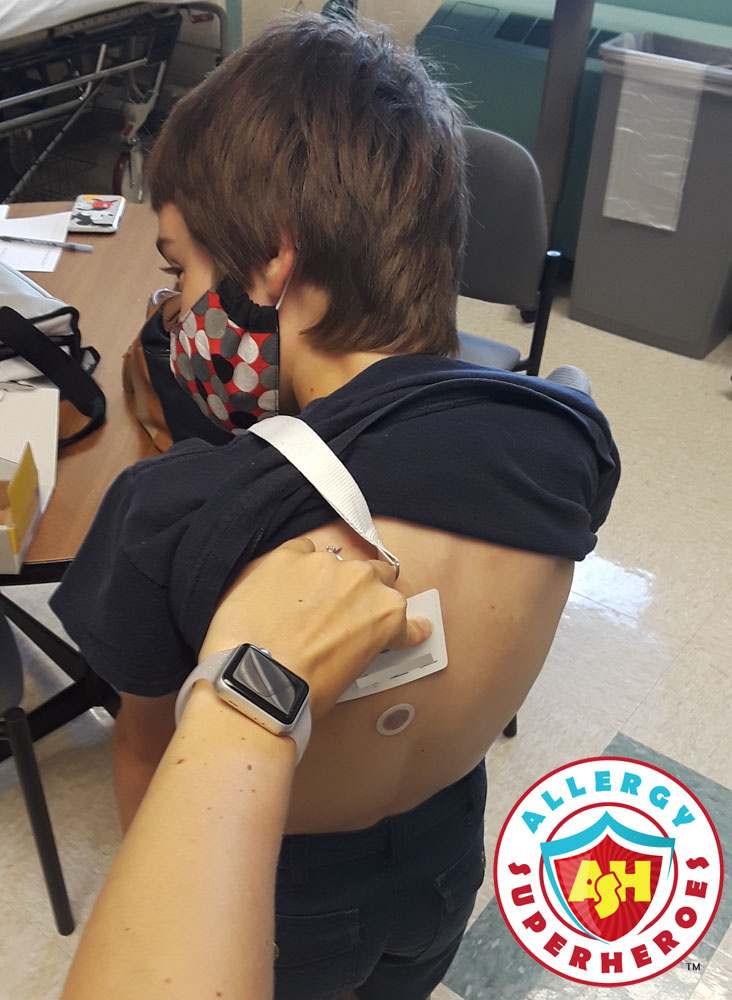
Since continuing the patch was not possible, our options were to do nothing and continue strict avoidance, or to do a food challenge and see if he had enough tolerance to transition into oral peanut dosing.
Oral Immunotherapy
As I briefly discussed before, Oral Immunotherapy (OIT) is the process of desensitizing the allergic person by eating gradually increasing doses of the allergen. Once the patient reaches a desired level of tolerance, they have to continue eating a “maintenance dose” daily in order to keep their tolerance. It should be noted that this should only be done under strict doctor supervision, as reactions are possible.
Our doctor was hoping that the patch had already given Kal a larger tolerance, so we could start higher than with traditional OIT. He envisioned us only “updosing” a couple of times and then maintaining tolerance.
I should note that I’ve known about OIT for years, but I’ve never pursued it for myself or for my children. There are several reasons.
My Feelings on OIT
The first is that it is not widely available. Most allergists are wary of the process. A few years ago, there was only one doctor in Colorado who would do OIT. He was more than an hour away, and he only did peanut.
(There are more doctors doing OIT now because of Palforzia. Palforzia is a standardized peanut OIT that doctors can now prescribe (as opposed to just using peanut products from the grocery store, which is what all OIT docs did before.) Palforzia was kind of in a race with DBV to achieve FDA approval. Obviously, Palforzia won.)
OIT is also very time-consuming. Because of the risk of anaphylaxis to doses, the initial dose has to be done in the office. So does every up-dose (when increasing how much the patient consumes.) The patient has to stay for a lengthy observation period after dosing as well.
OIT also has a high risk of reactions. Minor symptoms are common following dosing, but anaphylaxis is also possible. It’s even possible to develop Eosinophilic Esophagitis (EOE) to the allergen you are trying to tolerate. That one concerned me.
Finally, OIT puts heavy restrictions on activity. Years of clinical trials for OIT, plus data from doctors in private practice, have shown that chances of anaphylaxis to the dose increase dramatically if the patient’s body temperature rises following the dose. This means that for 2-3 hours after dosing, a patient has to stay “low key” because exercise or physical activity can increase body temperature too much. Even being out on a hot summer day or getting in a shower or hot tub can be enough to tip the balance.
Turn offs
This “rest period” has always been my biggest turn-off for OIT. After all, you don’t want to dose right before school, because you don’t want the burden of monitoring minor symptoms to be on the school staff. And you don’t want to dose right before bed, because anaphylaxis might make the child unable to call for help if they are alone in their bedroom. So finding a three-hour window between school and bed where the child is awake but able to stay relaxed is not easy.
I knew all of this in advance, and I asked our study doctor if the same rest period and reaction risks would apply to peanut dosing following the patch. He said it would. Which I had figured, but I’d hoped we were somehow exempt. As I said, OIT has never appealed to me much.
But at the same time, we had already put three and a half years into the REALISE study. We didn’t want to just walk away from any tolerance Kal had gained. So daily oral dosing was our only option.
But first we had to do a food challenge to see if Kal’s tolerance was even in a good place for peanut dosing.
First Food Challenge
We actually had two options for the food challenge. We could have made the food challenge be the final act of the REALISE study–there was an optional exit challenge. Kal’s tolerance would then be a data point for DBV. Unfortunately, if we chose this route, Kal would have to eat the “goop,” and we would have to keep dosing him until he reacted. Considering what we knew of the “goop,” and of anaphylaxis in general, this option promised to be uncomfortable at best and traumatic at worst.
Our other option was to officially finish and exit REALISE, and then do a private food challenge. This is the option we chose. Our doctor suggested Reese’s Pieces as the medium for our challenge. He said they are easy to dose with and are generally accepted by kids (for both taste and texture.)
So I bought a box of Reese’s Pieces and two weeks after our “End of Treatment” visit, we returned for our “End of Study” visit. This visit was a basic checkup, but immediately following, we launched into Kal’s peanut challenge.
The plan was for Kal to only eat one dose. He’d eat two Reese’s Pieces, and then we would wait for 90 minutes for observation (longer if he presented with symptoms.) Two Reese’s Pieces was roughly equivalent to 100mg* of peanut protein.
Assuming that Kal passed the challenge, we would have him eat that dose daily for a minimum of two weeks. We’d return to the clinic after two weeks for an up-dose appointment, where he’d jump to 4 Reese’s Pieces (200mg*.) After another two weeks (minimum) he would up-dose again to 6 Reese’s Pieces (300mg*.) 300mg peanut protein is equivalent to one peanut. Then we would maintain that dose.

*This turned out to be wrong, keep reading.
First time peanut dosing
I knew Kal was nervous about eating peanut. A year before, he had declared that he would never do a food challenge, so I was very proud of him for giving it a try. Days before the challenge, he insisted that he would only try it with ice cream. Fortunately, the clinic had little cups of ice cream in their fridge, so they were able to accommodate his request.
They put two Reese’s Pieces in his little cup of ice cream and told him to make sure he chewed them up before he swallowed. When eating them, Kal said he thought they tasted good. He could still taste the peanut a few minutes later though, and didn’t like it as much anymore.
About seven minutes after eating the Reese’s, Kal reported that his tongue itched a little. The doctor and nurses looked him over and gave him some ice water, but then we went back to waiting. I knew that minor symptoms are common during OIT, so this was within the realm of normal.
Kal’s tongue itching extended to his throat a little, and he also reported some minor stomach upset. The latter diminished when he snacked. After our waiting period, Kal’s symptoms were disappearing and we did our final check-in with the doctor.
These symptoms were all common with oral dosing, he told us, and we were cleared to begin peanut dosing at home. Kal was supposed to eat his dose with a meal or large snack, and observe the “rest period” I mentioned above. If the symptoms (or “side effects”) were bothersome, we could shift the time of his daily antihistamine so that he would take it right before dosing. They also gave us their 24/7 phone number and a list of instructions on when not to dose, when to call the clinic, etc. Then they sent us on our way.





Peanut Dosing at Home
Our first day of home oral peanut dosing went great. Kal reported a few symptoms, but less severe than the day before, and he was easily distracted with Legos. Unfortunately, that didn’t last.
On day two of dosing at home, Kal did not tolerate his dose well. It began with the standard stomach pain, but this time the pain increased in intensity. At one point, he ran to the bathroom to poop. There wasn’t any diarrhea, but he said it came out so fast that it was painful. Then he rolled around on the floor saying how much his stomach hurt.
I’ve got to say, as a parent, that moment was really weird. We had reached a level of symptoms that would call for epinephrine under normal circumstances–but these weren’t normal circumstances. This wasn’t an accidental ingestion, he’d eaten it on purpose. Some symptoms were expected. So where was the line?
In our exit instructions, severe stomach pain was listed as a reason to call the clinic’s 24/7 phone line, so I did. After listening to the situation and asking a few questions, they instructed me to dose him with liquid antihistamine and to keep monitoring him. If any further symptoms appeared, we were to Epi. They also said they would report his reaction to the doctor, who would call me back later to follow up.
A lengthy reaction
I gave Kal liquid Benadryl (the only liquid antihistamine I had in the house) and then kept an eye on him. He wanted to watch YouTube, so I had him do so on my old phone, on the floor of the living room. I didn’t want him watching on the TV in the basement, because then I wouldn’t be able to see him.
After a while, Kal reported feeling a little better, but it was a slow recovery. It soon became hard for him to wait to feel better, because fun things started happening around him. This was still the end of summer, and soon one of his neighborhood friends came knocking on the door, wanting to play. I told Kal I didn’t want him going out until he felt better.
Twice over the next few hours, Kal declared that he felt well enough to play. In both cases, he went outside for a few minutes. I told him he had to stay within the bounds of our yard and immediate vicinity, in case he needed help or I needed to find him. And in both cases, he came back in within a few minutes with a resurgence of stomach pain.
Kal’s stomach pain ebbed and flowed for the rest of the day. I even gave him a second dose of Benadryl four hours later. By the time he went to bed, thoroughly exhausted from a long and rough day, I was doubting myself. Sure, the severe stomach pain had never been life-threatening, nor had he experienced any further symptoms. But I couldn’t help but wonder if we’d have nipped the whole thing in the bud quickly if we’d just Epi’d.
Next Steps for Peanut dosing
When I spoke to the doctor later, he was surprised at how long Kal’s reaction had lasted. He told me I could have done it either way, and Epi might have made him feel better sooner. He even pointed me to FARE’s updated action plans for COVID-19. If it was just stomach pain, we could have Epi’d and not worried about going to the E.R. unless further symptoms developed. I decided that if this were to happen again, that’s what I would do.
But this reaction also brought about the question: “what do we do next?” The doctor told us that we probably ought to lower the dose. We could try just one Reese’s Piece at home the following day, or we could come back in for another food challenge to one Piece before resuming at-home peanut dosing. Or we could declare that we’d had enough, and walk away.
Considering our 3 1/2 year commitment already, I still didn’t want to walk away just yet. Kal agreed, but declared that he wanted another in-office challenge when he tried it again. And so, a few days later, we returned to the clinic for another challenge.
Second Peanut Challenge
We returned to the office the following week. Before we began, the doctor told us that they’d been in further contact with Reese’s, and he had updated information for us. It turned out that one Reese’s Piece contained 85mg of peanut protein–not the 50mg they’d been told before. 3.5 pieces were equivalent to one peanut. This also meant Kal had been eating more than half a peanut the previous few days of dosing–more than we’d intended to try.
So we would challenge and dose Kal with one Reese’s Piece. The doctor thought we also ought to slow down our up-dose schedule to make sure his body had time to adapt. There was no rush to up-dose quickly.

Kal’s second peanut challenge went much the same way as the first. About 7 minutes after eating the Reese’s (once again in ice cream), he began to feel some itching in his mouth, followed by stomach pain.
His symptoms all remained relatively mild. However, they kept us for a longer observation. Considering his previous reaction, the doctor wanted Kal’s symptoms to be completely cleared up before we left, just to make sure. This made for a long morning, with both of us getting increasingly hungry.
But finally, we were able to go home, with the instructions to dose with one Reese’s Piece every day. Kal’s next convenient day off from school was in 6 weeks, so that was when we scheduled his next up-dose. We planned to up-dose more slowly too–only increasing one Reese’s Piece each time, until we reached maintenance.
Peanut Dosing at Home Again
So we began home peanut dosing again. School started, so finding a three-hour window where he could mostly rest was harder, but as long as we were strict about dinner time, we managed to have him dose with dinner and be awake and restful for the required hours.
We discovered first-hand how activity and a hot shower should not be done in that three-hour window. On one day, Kal went out to play after dinner. Even though I had told him he couldn’t bike or run around, he had to just walk, talk, and stay mostly still during his play, I think he probably forgot that advice.
He still did okay until it was time for him to come in and take a shower. Following that, his stomach pain got worse. Not as bad as the day I considered using epinephrine, but still worse than “usual.” After that, we had to rearrange our schedule so that he would shower before dinner.
One would think that we’d already experienced enough bumps in the oral peanut dosing road, but unfortunately, that wasn’t to be the case. Next up will be our next dosing complication, and what followed.